Epidemiological Studies
There are now over 40 reports and studies in undeveloped societies who do not or did not have access to salt. These societies have low blood pressure compared to developed societies and no rise in blood pressure with age. Whilst there may be other factors that also account for the lower blood pressure, several studies have clearly demonstrated the profound importance of salt intake alone. For instance, a study in the Pacific Islands where one undeveloped community used seawater in their food and the other did not showed the community using seawater had higher blood pressure (1) . Another study in Nigeria of two rural communities, one of which had access to salt from a salt lake and the other did not, showed differences in salt intake and differences in blood pressure, and yet in all other aspects of lifestyle and diet the two communities were similar. The Qash'qai, an undeveloped tribe living in Iran who have access to salt deposits on the ground, develop high blood pressure and a rise in blood pressure with age similar to that which occurs in western communities, but in all aspects live a lifestyle similar to undeveloped communities who do not have access to salt (2) .
In spite of this evidence, it was felt necessary to set up a carefully controlled study of 52 communities throughout the world - the InterSalt Study (3) - with individual measurements of blood pressure, weight and 24 hour urinary sodium and potassium. The intention was to study communities with a wide range of salt intake, ie from 0.5 grams per day to 25 grams per day.
However, only four communities studied had a low salt intake (ie 3 grams per day or less) and the rest lay between 6 and 12 grams of salt per day and none had the high salt intake as originally envisaged. Nevertheless, the study showed there was a positive relationship between salt intake (as judged by 24 hour urinary sodium excretion) and blood pressure. There was also a positive and highly significant relationship between the increase in blood pressure with age and salt intake (Fig 1). This relationship showed that an increase in 6 grams of salt per day over 30 years would lead to an increase in systolic pressure in the whole population by 9 mmHg (3).
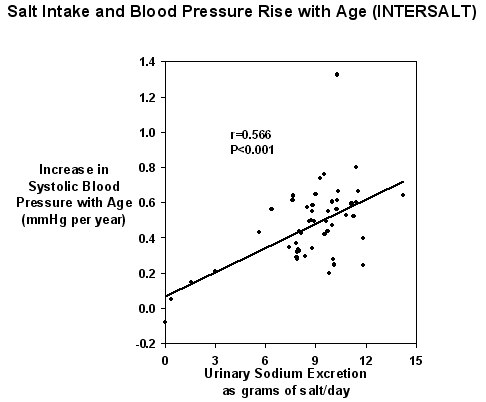
Figure 1. The relation of salt excretion to the slope of the rise in systolic blood pressure with age in 52 centres in the INTERSALT study. (Adapted from Ref. 3 ).
One criticism of the InterSalt study made by the Salt Institute (a public relations company defending the interests of salt extractors and manufacturers worldwide) was that when the four communities consuming less salt were excluded, there was no overall relationship remaining between salt intake and blood pressure in these 48 communities. Subsequently, the Salt Institute published a paper criticising the statistics of the study. The InterSalt Study's authors re-analysed their data and the results were published simultaneously (4). The conclusion was that the re-analysis strengthened the original InterSalt results and their conclusions still stood that salt intake was related to blood pressure throughout different populations in the world, and that there was a robust relationship between salt intake and the rise in blood pressure with increasing age.


