Treatment Trials
Studies, since the early 1900s, have shown that in those subjects with high blood pressure, restricting salt intake causes large falls in blood pressure. The classic studies of Kempner clearly showed major effects, even in very severe hypertension (1).
More recently, more modest reductions in salt intake, i.e. to around 5 to 6 grams per day from an intake of 10 to 12 grams per day, have been shown to cause falls in blood pressure in hypertensives equivalent to single drug therapy (2). These falls are larger in those subjects with lower levels of plasma renin activity or angiotensin II, for example those of African origin (3, 4) or older subjects. Furthermore, modest reductions in salt intake have been shown to be additive to drug treatment (5).
A double blind study of salt reduction with three salt intakes - 12, 6 and 3 grams per day in subjects with mild untreated essential hypertension showed a clear dose response to the salt reduction with large falls in blood pressure on 3 grams of salt per day (6). Furthermore blood pressure remained controlled on the lower salt intake at one year of follow up. Three longer term studies from the USA have also demonstrated that quite small reductions in salt intake not only lower blood pressure, but may also prevent the development of hypertension, and may allow the withdrawal of drug therapy (7).
A double-blind study in older subjects demonstrated that the fall in blood pressure in normotensive individuals with a modest reduction in salt intake from 10 to 5 grams of salt per day, was the same as those with high blood pressure (8). This suggested a large potential benefit of salt reduction in preventing strokes in this vulnerable elderly group who have blood pressure in the upper range of normal.
More recently, the DASH Sodium Study, a well controlled feeding study, has clearly demonstrated that reducing salt intake lowers blood pressure substantially, not only in hypertensives but also in normotensives, and importantly there was a dose-related response (4). Furthermore, there was a further fall in blood pressure with the salt restriction when a separate group of patients were fed a DASH diet consisting of more fruit and vegetables and less saturated fat. This study is of importance in that it demonstrates that not only would there be benefit from reducing salt intake on the diet that we currently consume, but there would be additional effects of restricting salt intake and consuming more fruit and vegetables and reducing saturated fat intake (Table 1 , Figure 1).
Table 1. Fall in blood pressure with salt restriction alone or the combination of salt restriction DASH-diet in hypertensive and normotensive individuals in the DASH-Sodium study.
|
|
Hypertensives (n=169) |
Normotensives (n=243) |
|
Salt restriction alone |
8.3/4.4 mmHg |
5.6/2.8 mmHg |
|
Salt restriction + DASH diet |
11.5/5.7 mmHg |
7.1/3.7 mmHg |
In spite of the clear results of the DASH Sodium study and the very carefully controlled double blind studies, some controversy has surrounded the effect of modest salt reduction in those with "normal or average" blood pressure. Meta-analyses of a variety of studies that have been undertaken in normotensives have shown small, but consistent, reductions in systolic pressure (9). Two recent meta-analyses of the effect of salt restriction on blood pressure showed that whilst the fall in blood pressure was significant in normotensive subjects, it was, according to the authors, of insufficient degree to be of public health importance (10, 11).
Close examination of these two meta-analyses shows that they are seriously flawed as they included many normotensive studies where salt intake had only been reduced for five days and there were very large reductions in salt intake, e.g. from 20 grams per day to less than 0.5 grams of salt per day over five days. This is known to cause stimulation of the sympathetic nervous system and brisk activation of the renin-angiotensin system (12). These very short acute reductions in salt intake are not relevant to the public health recommendations of a more modest reduction in salt intake from 10-12 grams per day to 5-6 grams per day, and in no way would the blood pressure lowering effect of a drug be judged over only five days of treatment.
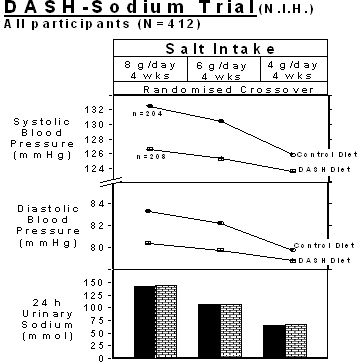
Figure 1. Changes in blood pressure and 24 h urinary sodium excretion with the reduction in salt intake in all participants (hypertensives: n=169; normotensives: n=243) on the normal American diet (i.e. control diet) and on DASH diet. (Redrawn from Ref. 4 ).
A more recent meta-analysis looked only at studies of one month or more in duration and only included studies with modest reductions in salt intake similar to the public health recommendations. This meta-analysis demonstrated a significant fall in blood pressure, both in systolic and diastolic blood pressure, not only in hypertensives but also in normotensive individuals (9) (Figure 2).
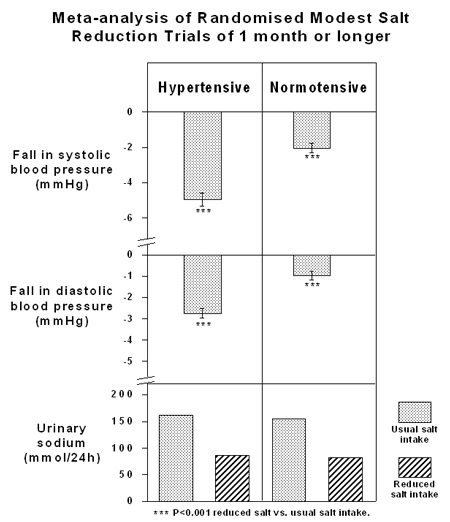
Figure 2 . Effect of modest salt reduction on blood pressure in hypertensive and normotensive individuals in a meta-analysis of 28 randomised controlled trials of 4 or more weeks. (Note average salt intake was reduced from 10 to 5 grams/day). (Adapted from Ref. 9).
The meta-analysis also showed a dose response so that a 6 gram reduction in salt intake would result in a fall in systolic blood pressure in the normotensive subjects of 4.0 mmHg (13) (Figure 3).
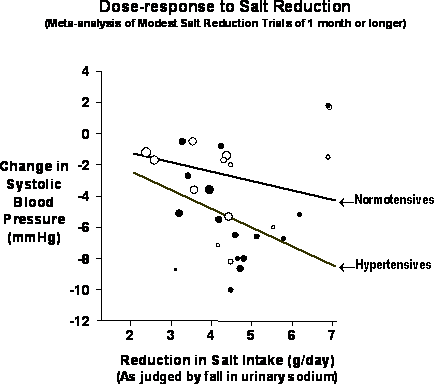
Figure 3 . Dose-response relationship between the reduction in salt intake as judged by reduction in 24h urinary sodium and systolic blood pressure. (Adapted from Ref 9).
It was concluded from the meta-analysis that a reduction of 6 g/day in salt intake, through the fall in blood pressure that would ensue, would lead to a reduction in stroke deaths of 24% (i.e. one-quarter), and ischaemic heart disease death of 20% (i.e. one-fifth) (13). Approximately, half of those affected by a stroke or heart attack die in the UK the population is approximately 60 million, there are 10.13 deaths/1000 population, and there are 240,000 deaths from cardiovascular disease each year. The average age is approximately 24 yrs, whereas in the UK the average age is 39 yrs. As the average age of a population increases so too does the percentage of the population affected by cardiovascular disease.
Most studies in the meta-analysis mentioned have been for one month only and it is likely that a longer duration of salt reduction would have a greater effect, particularly if it also prevented or slowed down the rise in blood pressure with age. The meta-analysis is also likely to under estimate the fall in blood pressure, as illustrated by the much larger falls in blood pressure that were seen in the very well controlled DASH Sodium study and the other double blind studies of salt reduction.
Please click on the following link to view a copy of a meta-analysis of randomised trials, published in the Cochrane Library (14), demonstrating that a modest reduction in salt intake has an important effect on blood pressure in both individuals with normal and elevated blood pressure - Cochrane Library meta-analysis for salt reduction [PDF 373KB]


